Whenever someone comes for diabetic foot care for the first time, they’re nervous and unsure. Often they’re thinking about pictures they’ve seen and stories they’ve heard of people with diabetes having foot and leg amputations. Of course, this can be very frightening. Fortunately, amputations aren’t a foregone conclusion when a person has diabetes – they are often avoidable.
The ‘-opathies’ of diabetes.
Diabetes includes three types of ‘-opathy’ – retinopathy (eyes), nephropathy (kidneys), and peripheral neuropathy (nerves). This means that the health of eyes, kidneys and nerves (among other things) are all at risk of impact from diabetes. And these can have an influence on lower extremity/foot health. When vision is impaired, caring for feet becomes difficult, and even dangerous. Poorly functioning nerves can create numbness, pain and tingling in feet, which makes walking challenging, but greatly increases risk of injury, which can lead to ulcers, which can lead to infection, which can lead to amputation…
Diabetic peripheral neuropathy
The phrase ‘diabetic peripheral neuropathy’ describes numbness, pain and tingling in feet that occurs as a result of diabetes.  Sometimes this can begin as feelings of pins and needles, or the sensation of little ants crawling on your feet. What happens is this: poorly controlled blood sugar levels cause nerves to become damaged. And where the damaged parts of the nerves are, the nerve impulses become sort of trapped. One way to understand this better is to picture a train on a track, coming up to a bridge. If the bridge is intact, the train can continue on its way. If the bridge is out, the train is stuck. So if the track is a nerve, and the train is the nerve impulse, you can see why if there’s damage to the nerve (the bridge is out), the impulse becomes stuck. As the impulse keeps trying to cross the bridge, but can’t, it starts to feel like a zap, or little shots of pain in that area. All the nerves past that point don’t get the impulse, which is what creates numbness. When an area is numb, injury happens very easily.
Sometimes this can begin as feelings of pins and needles, or the sensation of little ants crawling on your feet. What happens is this: poorly controlled blood sugar levels cause nerves to become damaged. And where the damaged parts of the nerves are, the nerve impulses become sort of trapped. One way to understand this better is to picture a train on a track, coming up to a bridge. If the bridge is intact, the train can continue on its way. If the bridge is out, the train is stuck. So if the track is a nerve, and the train is the nerve impulse, you can see why if there’s damage to the nerve (the bridge is out), the impulse becomes stuck. As the impulse keeps trying to cross the bridge, but can’t, it starts to feel like a zap, or little shots of pain in that area. All the nerves past that point don’t get the impulse, which is what creates numbness. When an area is numb, injury happens very easily.
So now what?
First things first. If you’ve been diagnosed with diabetes, be sure to follow up with your doctor, nurse practitioner or Certified Diabetes Educator. Above all, listen to them – they’re the experts. Refinements to lifestyle and diet, and taking your medication as prescribed will stand you in good stead. Ensure you have honest, open conversations with your health care provider(s). They aren’t mind-readers, and rely on you to provide accurate information.
Caring for your feet
Monitor your feet daily. If you can’t reach your feet to see them, invest in a hand-held mirror to help.  Look for any injuries, splinters or slivers, or skin changes. If you can’t see your feet but can reach them, feel your feet with your hands. Monitoring your feet regularly will alert you to anything which may require medical attention.
Look for any injuries, splinters or slivers, or skin changes. If you can’t see your feet but can reach them, feel your feet with your hands. Monitoring your feet regularly will alert you to anything which may require medical attention.
If you can reach your feet, and can see what you’re doing, trim your toenails carefully with a straight-edged nail clipper, straight across. If your toenails are thicker than the opening of the clipper, don’t force it. Arrange a visit to our St. Catharines foot clinic or chiropodist for help. Please don’t get creative with garage tools or utility knives. The risk of injury is very high when you depart from using instruments designed for use on living tissue.
Care for calluses carefully, gently rubbing them with a pumice stone lubricated with a little bar soap, every few days, and follow with application of a callus cream. This kind of cream is designed specifically for calluses and often contain urea. Urea helps to keep the production of callus cells down to a minimum. Apply callus cream nightly, being sure to have slippers handy if you need to get out of bed for any reason. Feet with cream on them can be slippery!
What does a foot care nurse do?
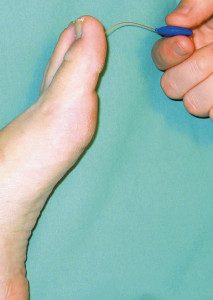
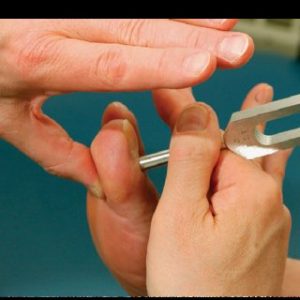
Great question! A foot care nurse will first assess, and then care for your feet. This will include them looking closely at your feet, inspecting your toenails and skin, assessing the range of motion in your feet, toes and ankles, as well as sensation testing, with either a 10g monofilament, or a tuning fork. Both of these tests are easy and painless, and help to establish and monitor any peripheral nerve involvement. The nurse can tend to toenails, calluses, skin cracks, or corns. They will also speak with you about caring for your feet with diabetes. Don’t be shy – ask questions! They’re your feet!
What to do if you injure your feet
 Apply first aid and seek prompt medical attention as necessary. Keep the injury clean and protected with a bandage, and monitor for signs of infection. Redness, swelling, heat, pain and discharge are the cardinal signs of infection. If you notice any one or more of these, call your doctor immediately. If you can’t see your feet very well and have a splinter/sliver, ask for help to remove it – please, NO DIY home surgery!
Apply first aid and seek prompt medical attention as necessary. Keep the injury clean and protected with a bandage, and monitor for signs of infection. Redness, swelling, heat, pain and discharge are the cardinal signs of infection. If you notice any one or more of these, call your doctor immediately. If you can’t see your feet very well and have a splinter/sliver, ask for help to remove it – please, NO DIY home surgery!
Some parting thoughts
Having diabetes doesn’t mean you’ll have to have an amputation. It means you’re at higher risk for developing ulcerations or injuries, perhaps because of nerve damage or poor blood sugar management. With careful glucose management, attention to lifestyle and diet and taking your medications, you can reduce the risk of lower extremity problems. Monitor your feet daily, get to know them. Know what they look like on a daily basis, so you’re immediately aware of any changes. Visit your local foot care nurse regularly. They are an important part of your health care team, dedicated to helping you keep your feet healthy.